The Key Takeaways
✓ Omega-3s lower triglycerides by 20–30% at 2–4 g/day, but the cardiovascular benefit goes beyond triglyceride lowering.
✓ Formula matters. EPA-only or EPA-dominant formulas are more effective in reducing cardiovascular events than EPA+DHA combinations (Sheppard 2025 meta-analysis: 21% vs 8% mortality reduction). The mechanism is still being worked out.
✓ High-risk patients defined as coronary calcium score >100, established atherosclerotic disease, or on statin therapy with TG >150, benefit most.
✓ There is no clear benefit in low-risk patients. If you don’t have risk factors, check an Omega-3 Index; aim for >8%.
✓ High-dose EPA carries a small but real atrial fibrillation risk (~1 percentage point absolute increase in REDUCE-IT). Worth knowing before self-prescribing.
✓ The FADS1 gene changes how efficiently your body converts plant omega-3s to EPA. Slow-converting (TT) carriers likely need preformed marine EPA to reach therapeutic levels.
In This Issue
Catch up on the rest of the series: Welcome to Pareto Life · Upcoming Series on Omega-3 · Issue 02 — Do Omega-3s reduce risk of dementia?
Want to know the science? Keep reading below 👇
Does fish oil actually prevent heart attacks? Most people assume yes…fish oil is one of the most-recommended heart supplements in the world, and social media has the generic “fish oil is good for your heart” message peppered all over the internet. But the clinical trial evidence is more divided than the supplement aisle suggests. Pure EPA worked dramatically in REDUCE-IT, cutting major cardiovascular events by 25%. EPA+DHA combinations at the same dose failed in STRENGTH. Who actually benefits, what dose, and which formula. Those answers depend on your risk profile, your triglycerides, and even a single gene called FADS1.
The research into benefits of fish oil benefits stemmed from an observation that indigenous people in Greenland had a low risks of heart disease, despite diets extremely high in fat from marine animals. This has lead to extensive research into the potential benefits of fish oil or Omega-3s fatty acids comprise of EPA and DHA.
How Fish Oil Affects Your Heart
It Lowers Triglycerides (TG) — Reliably
Elevated TG are linked to heart disease. At doses of 2-4gm per day, EPA and DHA have demonstrated consistently in studies to reduce TG by 20-30%.
It Fights Inflammation — Sort Of
Omega 3s and Omega-6 Fatty acids compete to be incorporated into the cell membranes. The incorporation of omega-3s into the cell membrane results in promoting pre-resolving mediators that act to resolving inflammation. At the same time by displacing Omega-6 from cell membrane results in inhibition NF-KB, a key mediator of inflammation.
It May Help Artery Health
The evidence is suggesting that Omega-3s may help with dilation of blood vessels and stabilization of plaque buildup in arteries.
⚠ What It Doesn't Do: Fix Your Cholesterol
Omega-3 has little or no overall effect on LDL. The 2020 Cochrane review confirms with high certainty that long-chain omega-3 (EPA+DHA) has little or no effect on LDL cholesterol, but DHA specifically tends to raise LDL across various populations. The increase in LDL includes favorably shifting LDL toward larger, less atherogenic particles and reducing small dense LDL, whereas EPA alone does not raise LDL. This differential effect helps explain why EPA-only formulations like icosapent ethyl (Vascepa) showed a cleaner lipid profile in REDUCE-IT, though EPA's cardiovascular benefits likely extend beyond lipids to anti-inflammatory and membrane-stabilizing effects.
What the Major Heart Trials Actually Show
EARLY POSITIVE TRIALS
The GISSI-Prevenzione trial (1999) is often cited as showing a 30% reduction in cardiovascular mortality with 1 g/day EPA+DHA in post-heart-attack patients. Important framing: the 30% comes from a four-way per-group analysis. The more conservative, pre-specified two-way analysis showed a 17% reduction. The Japanese JELIS study showed EPA added to statin therapy reduced major coronary events by 19%, though JELIS was open-label without a placebo, which limits how confidently we can attribute the effect to EPA itself.
REDUCE-IT (2019)
8,179 high-risk patients · Elevated triglycerides · On statin therapy
4 g/day of highly purified EPA (icosapent ethyl) reduced major adverse cardiovascular events by 25%, including reductions in cardiovascular death, heart attack, stroke, and revascularization. Post hoc analysis suggest the impact of Omega-3s may be independent of baseline triglycerides.
VITAL (2019)
25,871 primary prevention participants · Largest omega-3 trial to date
Low-dose EPA+DHA (840 mg/day) showed no significant reduction in primary cardiovascular events.
ASCEND (2018)
15,480 diabetic patients · 840 mg/day EPA+DHA
Failed to reduce serious vascular events overall, though exploratory analyses suggested a 19% reduction in vascular deaths.
STRENGTH (2020)
Similar population to REDUCE-IT · 4 g/day EPA+DHA combination
Terminated early for futility with no cardiovascular benefit despite the high dose — highlighting that EPA-only formulations may outperform combined EPA+DHA.
It's Not Only About the Dose — It's the Formula
Here's where it gets interesting. REDUCE-IT (pure EPA, 4g/day) worked great. STRENGTH (EPA+DHA combo, same 4g/day dose, nearly identical patient population) failed completely. Why?
There are many theories. First, the placebo used in REDUCE-IT was mineral oil and in the STRENGTH trial was corn oil. Unlike corn oil, mineral oil did result increase CRP and LDL-C in the REDUCE-IT trial, which could increase the risk of cardiovascular outcomes. However, even after accounting for this explanation, there was still a 25% risk reduction. Another potential explanation is related to DHA. Adding DHA to EPA might actually cancel out EPA's benefits. A 2025 meta-analysis of 127,771 patients compared EPA to EPA+DHA formulations and EPA-only reduced cardiovascular mortality by 21% compared while EPA+DHA reduced it only by 8%.
Why Does DHA Blunt EPA's Benefits?
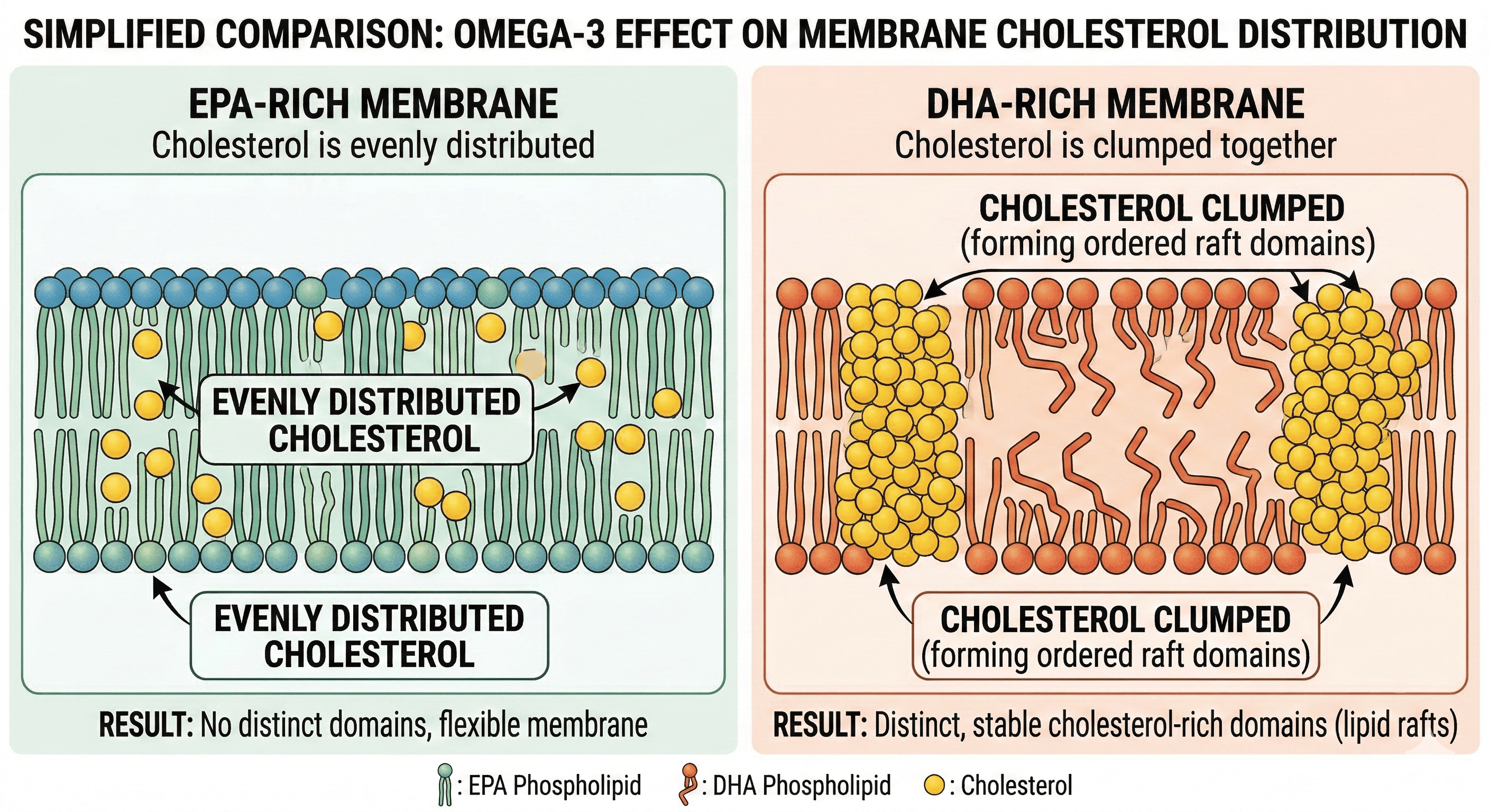
The structure of EPA is compact and stable and therefore when it is incorporated in the cell membranes its keeps cholesterol evenly distributed. However, DHA is larger and more flexible which helps with cell membranes fluidity and flexibility but also can cause cholesterol to clump together in concentrated pockets.
In artery plaques, where cholesterol is already a problem, EPA tends to stabilize plaques. DHA may increase cholesterol crystal formation.
A 2025 analysis of 16 trials (127,771 patients) found pure EPA reduced cardiovascular death by 21%, while EPA +DHA formulations only reduced it by 8%.
REFERENCES[1] Nicholls SJ et al. JAMA 2020 (STRENGTH trial). [2] Nissen SE et al. JAMA Cardiol 2021. [3] Sherratt SCR et al. Cardiovasc Res 2024. [4] Sheppard JP et al. JACC Adv 2025. [5] Chapman MJ & Mason RP. Pharmacol Ther 2022. [6] Sherratt SCR et al. Curr Atheroscler Rep 2022.
Your Genes Affect How Well Fish Oil Works for You
Think of your genes like a factory that converts plant-based omega-3s into the more powerful EPA your body actually uses. The FADS1 gene controls how well that factory runs.
Converting plant omega-3s to EPA (e.g. from flaxseed, walnuts, chia):
• CC genotype = Fast factory: Your body is better at converting plant omega-3s into EPA. When people with CC genotype ate more plant omega-3s (ALA), their blood EPA rose by 2.2%.
• TT genotype = Slow factory: Your body struggles to make this conversion which may result a deficiency of EPA . The same increase in plant omega-3s only raised blood EPA by 0.9% — less than half the response of CC types.
What Your Genotype Means in Practice
People with the CC genotype (higher enzyme activity): For every unit increase in dietary EPA, circulating EPA rises by ~3.7%. While people with the TT genotype (lower enzyme activity), the same unit increase raises circulating EPA by ~7.8%.
For TT carriers, omega-3 supplementation may actually have an outsized impact for two related reasons. First, because the FADS1 conversion factory runs slowly, TT carriers make less EPA from plant-based omega-3s, and thus these carriers may have a lower baseline status. Second, that same slow factory also produces less arachidonic acid, the omega-6 fatty acid that normally competes with EPA for spots in cell membranes. As a result, it is possible that each gram of supplemented EPA likely does more work in a TT carrier than in a CC carrier.
Practical takeaway: if you are a TT carrier, plant omega-3s alone (flaxseed, walnuts, chia) are unlikely to bring your EPA into the therapeutic range, because the enzyme that makes this conversion is inefficient. You likely benefit from fish oil or Omega3 to overcome the slow conversion. CC carriers convert more efficiently from plant sources but still derive cardiovascular benefit from preformed marine EPA when the goal is high circulating EPA.
If you’re healthy check your Omega-3 Index
Instead of guessing how much fish oil you need, there's actually a blood test you can take. It's called the Omega-3 Index, and it measures EPA+DHA as a percentage of your red blood cell fatty acids.
This tells you not just how much omega-3 you're consuming, but how much is actually getting into your cells. As a physician, I like to measure efficacy of treatment.
OMEGA-3 INDEX | RISK LEVEL | INTERPRETATION |
|---|---|---|
Below 4% | High Risk | Strongly associated with elevated CVD mortality risk |
4% – 8% | Intermediate | Opportunity for meaningful improvement |
8% – 11% | Target Range | Associated with lowest cardiovascular disease incidence |
Moving from a 4% to an 8% index is associated with ~30% lower risk of dying from coronary heart disease.
In the Framingham Heart Study (one of the longest-running heart studies ever), people in the top quintile for omega-3 index had 34% lower all-cause mortality and 39% lower cardiovascular disease compared to those with the lowest levels.
Safety: The Atrial Fibrillation Signal
One safety consideration to be reminded of: high dose EPA increase risk of atrial fibrillation, which is an irregular heart rhythm. In REDUCE-IT, hospitalizations for atrial fibrillation or atrial flutter occurred in 3.1% of patients on EPA versus 2.1% on placebo. The risks vs benefits of high dose omega3 should be discussed with your physician.
What if you are on a statin
Meta-analysis of 5 RCTs as well as the REDUCE-iT and JELIS trials demonstrated the benefit of high dose EPA (~2gm) in cardiovascular death, heart attack, stroke even when patients were on statins.
Who Benefits Most?
HIGH-RISK PATIENTS
If a person has any of the following health issues, there is strong evidence that omega-3s are beneficial.
• You've had a heart attack or stroke
• You're on statin therapy but still have elevated triglycerides (≥150 mg/dL)
• You have a high coronary artery calcium score (≥100)
• You have established atherosclerotic cardiovascular disease
INTERMEDIATE AND LOW-RISK PATIENTS
If you're generally healthy with no cardiovascular risk factors, the evidence for fish oil supplements protecting your heart is weak. My recommendation is to check your Omega-3 index to see if you are high risk and would benefit from supplementing.
Did you find the email helpful?
Coming up in future issues: how omega-3s affect your brain and cognitive health, their role in managing inflammation throughout the body, and a practical guide to choosing the right supplement for your individual profile.
References
Innes & Calder, Int J Mol Sci 2020 Elagizi et al., Nutrients 2021 Weinberg et al., JACC 2021 O'Keefe et al., Mayo Clin Proc 2019 von Schacky, Proc Nutr Soc 2020 Harris et al., Am J Clin Nutr 2008 Harris et al., Atherosclerosis 2017 Franco et al., J Clin Lipidology 2025 Nicholls SJ et al., JAMA 2020 Nissen SE et al., JAMA Cardiol 2021 Sherratt SCR et al., Cardiovasc Res 2024 Sheppard JP et al., JACC Adv 2025 Chapman MJ & Mason RP, Pharmacol Ther 2022 Sherratt SCR et al., Curr Atheroscler Rep 2022 Schulze MB et al., Lancet Diabetes Endocrinol 2020 Al-Hilal M et al., J Lipid Res 2013 Juan J et al., Am J Clin Nutr 2018, Doi T, European heart Journal, 2021. Sheppard JP, JACC 2025.